Emerging research since the COVID-19 pandemic began suggests that poor oral health may heighten infection risks. A U.S. study now reveals that patients with gum disease face significantly greater chances of severe outcomes.
Periodontitis, a chronic inflammatory condition, gradually erodes the tissues supporting the teeth. Often progressing from untreated gingivitis, it can lead to tooth loosening and loss. Evidence indicates that periodontitis and other oral conditions paired with COVID-19 pose serious threats.
Published in June 2021 in the Journal of Dental Research, a study found COVID-19 patients with gum disease were 3.5 times more likely to require intensive care, 4.5 times more likely to need mechanical ventilation, and nine times more likely to die from the virus.
Poor oral hygiene also raises secondary infection risks. Aggressive oral bacteria can travel to the airways and lungs via inhalation.
Researchers from the University of Brasília (Brazil) note that periodontitis elevates levels of the immune protein interleukin-6 (IL-6). This triggers gum inflammation that may impact lungs and blood vessels. Analysis of multiple studies showed patients with IL-6 levels above 80 picograms per milliliter faced higher risks of acute respiratory distress syndrome, often requiring ICU admission or respiratory support.
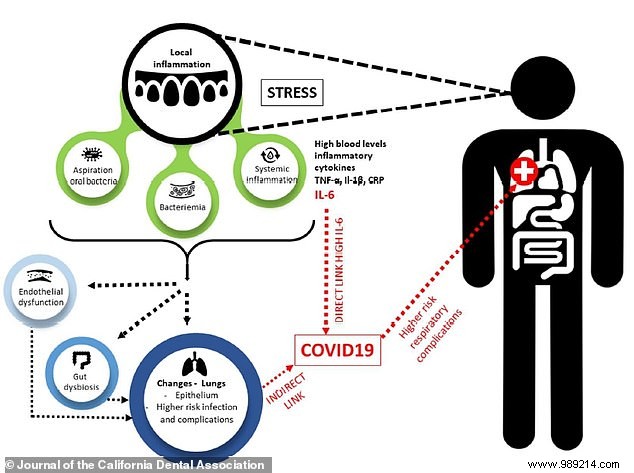
To combat aggressive bacteria from poor oral health, the body ramps up immune cell production, including IL-6. Those genetically predisposed to high levels often develop chronic gum disease. IL-6, one of the more harmful cytokines, contributes to bone and tissue destruction and impairs blood vessel dilation, potentially leading to hypertension.
As a cytokine, IL-6 plays a key role in the "cytokine storms" seen in severe COVID-19 cases—an immune overreaction linked to complications. Studies suggest the virus doesn't directly destroy lung tissue; rather, misguided immune responses cause the damage.