In recent years, innovative medical techniques like hypnosis have gained traction in healthcare, despite initial skepticism. Recognized by the World Health Organization (WHO) as a form of traditional and complementary medicine—alongside acupuncture and osteopathy—medical hypnosis is now used in therapy and surgical settings. Backed by clinical evidence, it helps manage pain and anxiety effectively. But how does it work, and which pains can it address?
Medically, hypnosis induces a heightened state of consciousness where external distractions fade, allowing deep focus. Therapists employ relaxation techniques, metaphors, and suggestion to alter pain perception—reducing sensations or even dissociating from them entirely. Extensive research supports its role in modulating how the brain processes pain signals.
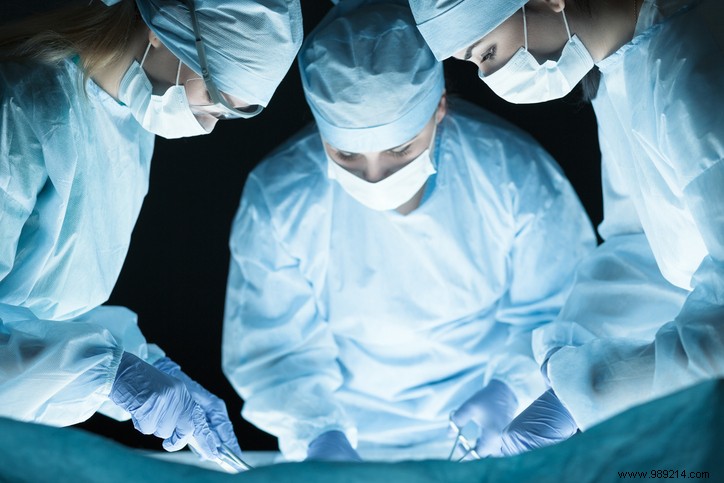
In surgical procedures, hypnosis minimizes the need for anesthetics and painkillers, speeding recovery and cutting costs. It's particularly valuable for patient comfort during operations. Primarily applied in surgery and psychotherapy, its benefits are increasingly validated by studies, including those from trusted sources like Doctonat, showing broad efficacy across pain types.

Hypnosis excels in medical settings, reducing pain, anxiety, and even bleeding during procedures. Studies on cataract and knee surgeries report significantly less intraoperative and postoperative pain compared to conventional methods.
Emerging innovations, like hypnosis combined with virtual reality, further enhance outcomes. For chronic conditions, it's proven effective against migraines, back pain, irritable bowel syndrome, and cancer-related discomfort.
Beyond physical pain, hypnosis aids psychological issues in clinical sessions, helping with smoking cessation, compulsive behaviors, and trauma recovery.
Enjoyed this? Explore more: