Osteoporosis primarily impacts people over 65, especially women. This condition progressively weakens and deforms bones as natural bone mass declines with age.
It commonly affects the spine, wrists, hips, pelvis, and shoulders, increasing the risk of fractures.
Advancing age is the leading cause, as it accelerates bone loss. In men, it typically emerges after 70; in women, often after 50, particularly post-menopause when declining estrogen levels speed up bone decalcification. Early menopause before age 40 heightens risk.
Heredity plays a key role, with 70-80% of bone mass determined genetically. Daughters of mothers with osteoporosis face double the risk.
Certain conditions, like rheumatoid arthritis, thyroid disorders, or kidney disease, can contribute to its development.
Lifestyle factors also matter: diets low in protein, calcium, and vitamin D; excessive coffee, alcohol, or tobacco use; and sedentary habits all elevate risk.
Known as the 'silent disease,' osteoporosis often progresses without pain or obvious signs until a fracture occurs, typically from a minor fall. Warning signs include vertebral compression fractures, leading to stooped posture (kyphosis) and noticeable height loss.
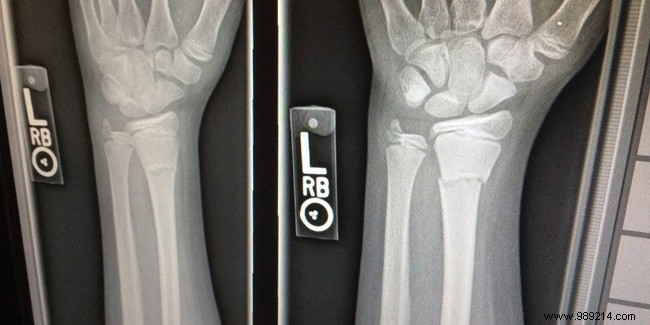
Diagnosis involves bone densitometry, a reliable scan measuring bone density.
A nutrient-rich diet is essential, delivering 1,000 mg of calcium daily and adequate vitamin D. Get vitamin D naturally through outdoor activity, as sunlight triggers skin synthesis—especially effective in summer. Calcium sources include milk, cheese, fish like sardines, leafy greens, dark chocolate, dried fruits, and calcium-rich mineral water.
Regular physical activity is crucial. Opt for low-impact exercises like walking, jogging, weight training, gymnastics, yoga, or water aerobics to build muscle strength, flexibility, and balance.
For diagnosed cases with high fracture risk, physicians prescribe medications that promote bone formation or reduce resorption. Hormone therapies may also be recommended to help preserve bone density.