Researchers led by Edward Morrisey at the University of Pennsylvania have identified a groundbreaking new type of cell in human lungs. These Respiratory Airway Secretory Cells (RAS) are essential for optimal respiratory function and show promise for treating smoking-related diseases.
Unlike mouse lungs, human lungs feature respiratory bronchioles where distal airways intertwine with alveolar gas exchange regions. This unique structure is absent in mice, leaving the cellular and molecular mechanisms of human respiratory bronchioles poorly understood.
Historically, studies have depended on mouse models, frustrating scientists due to anatomical differences.
In a recent study published in Nature, Morrisey's team used advanced single-cell gene analysis on healthy human lung tissue samples to uncover these RAS cells in the bronchioles.
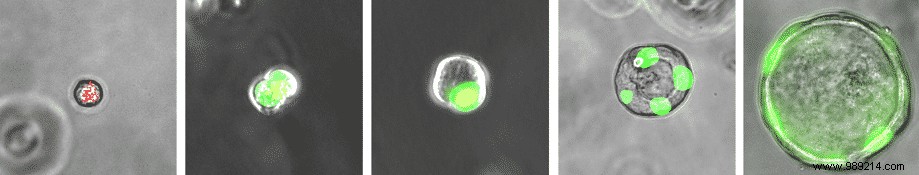
RAS cells serve two vital roles: they secrete molecules that maintain the protective mucus layer in bronchioles for efficient lung performance, and they act as progenitor cells. Like stem cells, they can differentiate into alveolar type 2 (AT2) cells, which produce surfactants to repair damaged alveoli.
Notably absent in mice, these cells appear in ferrets—whose lungs more closely resemble humans—and likely in other mammals of similar or larger size.
This discovery could transform treatments for chronic obstructive pulmonary disease (COPD), which involves progressive lung tissue degeneration, airway obstruction, and emphysema. Risk factors include smoking, childhood respiratory issues, and air pollution, impairing oxygen absorption.
RAS cells may naturally repair damaged alveoli in COPD, but factors like smoking likely impair them. Introducing functional RAS cells could enhance therapies or even cure the disease, pending further research.