Glaucoma is a progressive eye disease that damages the optic nerve, commonly linked to aging. It alters the visual field and can lead to partial or total blindness if untreated. As experts in eye health, we'll cover how to spot symptoms early and the most effective treatments.
According to the Federation of the Blind of France, nearly one million people—2% of the French population—live with glaucoma. Risk rises significantly after age 45.
Glaucoma affects the optic nerve through elevated intraocular pressure, compressing nerve fibers and gradually narrowing the visual field.
It disrupts the flow of aqueous humor, the clear fluid that maintains eye pressure and renews naturally. In open-angle glaucoma, drainage slows; in angle-closure glaucoma, it's blocked entirely.
Age is the top risk factor, with onset possible from 40-45 and increasing thereafter. Family history heightens vulnerability.
Nearsighted individuals, those with high blood pressure, diabetes, sleep apnea, or prolonged corticosteroid use also face elevated risks.
Glaucoma often progresses silently, with no early vision changes. Field loss develops slowly, which is why annual ophthalmologist exams from age 45 are essential for early detection.
Watch for eye pain, redness, blurred vision, or peripheral loss creating tunnel vision—seek care immediately.
Loved ones may notice struggles with reading, close-up TV viewing, clumsiness, light sensitivity, or behavioral shifts like irritability or withdrawal, sometimes mistaken for depression or Alzheimer's.
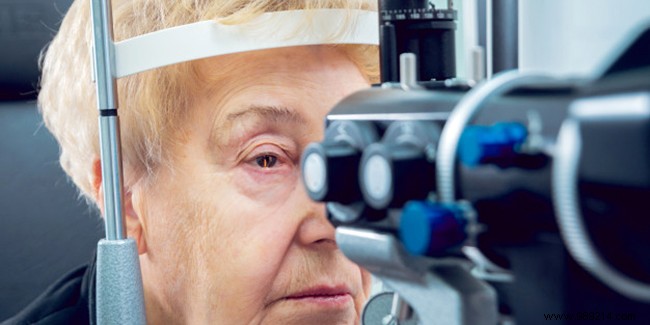
Diagnosis includes tonometry for intraocular pressure, ophthalmoscopy or OCT for the optic nerve, gonioscopy for drainage angles, and visual field testing. MRI may be ordered if needed.
No cure exists, but treatments effectively stabilize the condition by reducing eye pressure. Eye drops, targeting aqueous humor, are first-line therapy.
For insufficient response, outpatient laser treatment improves drainage or cuts production—though effects may wane, requiring drops later.
Surgery, as a final option, creates new drainage paths or limits production during a brief hospital stay or outpatient procedure.
Key Note: Stabilizing treatments, particularly surgery, raise cataract risk.