Hypertension, commonly known as high blood pressure, is a prevalent cardiovascular condition that often develops without noticeable symptoms. Yet, it poses significant risks, including stroke and neurodegenerative diseases. It affects about one in three adults, rising to 65% in those over 65.
Arterial hypertension (HTA) is a leading cardiovascular issue, impacting one in three adults—particularly older individuals—and is France's most common disease. It's a primary cause of strokes and contributes to complications like heart attacks and Alzheimer's disease.
Hypertension involves persistently elevated blood pressure, the force exerted by blood against artery walls as the heart pumps. Over time, this can thicken and stiffen arteries, forming atherosclerotic plaques that may block or rupture vessels.
Chronic high pressure also strains the heart, potentially leading to left ventricular hypertrophy and heart failure.
Blood pressure is assessed using two values: systolic (higher, during heart contraction) and diastolic (lower, during heart relaxation). Hypertension is diagnosed when systolic exceeds 140 mm Hg or diastolic exceeds 90 mm Hg.
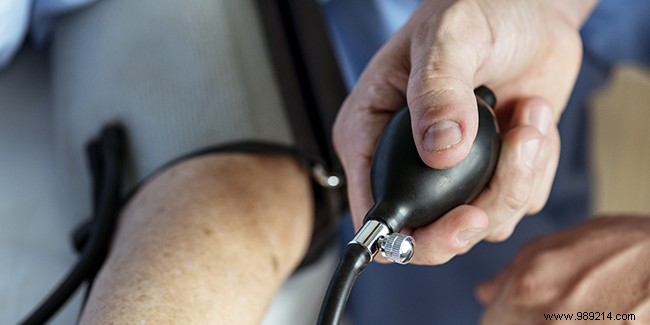
Doctors use a cuff at heart level for initial readings, but confirm diagnosis over multiple visits, as values fluctuate with time of day, activity, stress, or other factors.
Additional validation includes home self-monitoring (three times morning and evening for three days) or 24-hour ambulatory monitoring with a wearable device recording every 15 minutes.
Hypertension often progresses silently; only half of affected adults are aware. It's frequently discovered incidentally during routine checks.
Possible signs include morning headaches, dizziness, vision changes, palpitations, sweating, nosebleeds, malaise, or shortness of breath.
Primary hypertension lacks a single identifiable cause, but key risk factors include:
Other contributors: male gender, socioeconomic disadvantage, chronic kidney disease, premature birth, sleep apnea, stress, or family history.
Effective management prevents severe outcomes like angina, heart attack, peripheral artery disease, kidney failure, retinopathy, or Alzheimer's.
Lifestyle changes are first-line: adopt a diet rich in fruits and vegetables (low in animal fats), exercise regularly, achieve healthy weight, limit alcohol (<3 drinks/day for men, <2 for women), quit smoking, cap salt at <6g/day, and control diabetes/cholesterol. These can normalize pressure within three months.
If needed, medications include thiazide diuretics (promote water/salt excretion), calcium channel blockers (aid vasodilation), ACE inhibitors or ARBs (relax vessels), beta-blockers (reduce heart rate), or central agents (regulate brain signals).