Affecting about 1 in 4,500 women worldwide, Mayer-Rokitansky-Küster-Hauser (MRKH) syndrome—often shortened to Rokitansky syndrome—is a rare congenital condition where individuals are born without a uterus or vagina. Those affected face profound challenges in building a normal life, but medical advancements offer hope.
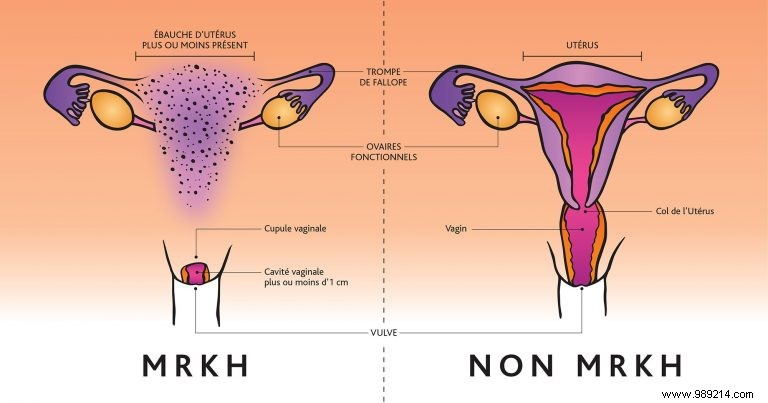
MRKH syndrome falls under differences of sex development, where a person's sex characteristics don't align with typical male or female definitions. It impacts women born without a vagina and uterus, though partial development can occur in some cases.
The condition develops in utero but is typically diagnosed during adolescence in 80% of cases. Take É lisa, featured in a Slate article on March 5, 2021: At 17, her gynecologist revealed she had ovaries and a partially formed vagina but no uterus—confirmed by an MRI prompted by absent periods despite developed secondary sex characteristics. The diagnosis: no possibility of pregnancy or vaginal intercourse.
Amélie Victor, president of France's MRKH Association, advocates for more research based on countless patient stories. Limited studies show it's caused by a gene mutation around the sixth week of embryonic development, halting Müllerian duct formation. While roughly 1 in 4,500 women are affected globally, the true prevalence may be higher.
Options include vaginal dilation (Frank's method), where patients use progressively larger dilators to form a functional vagina from their own tissue. With proper therapeutic support, this can yield a normal-sized vagina in about six months.
Surgical alternatives, like sigmoid graft vaginoplasty or the Vecchietti technique, are options, but experts note outcomes aren't always superior to dilation. Success demands strong psychosexual maturity and skilled medical teams.
These approaches can significantly enhance sexual function, though uterine absence prevents natural birth. Uterus transplantation, legalized in France in 2015, brings new possibilities. In 2019, Prof. Jean-Marc Ayoubi at Foch Hospital in Suresnes performed the country's first such procedure. Researchers are now tracking long-term outcomes, including embryo implantation, pregnancy, and live births, to confirm its viability.