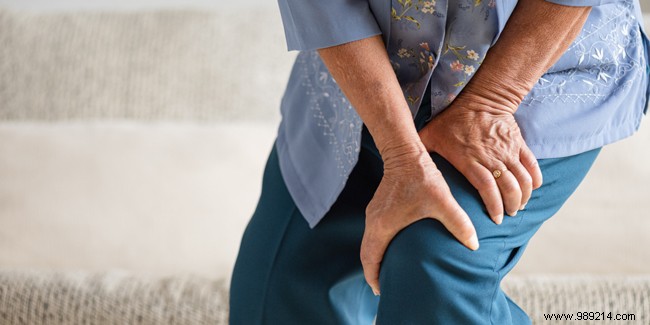
Joint pain becomes more prevalent with age, often referred to as polyarthralgia. These aches can range from uncomfortable to debilitating, significantly impacting daily well-being. Identifying the root cause is key to effective treatment. Explore the primary causes of joint pain, treatment options, and prevention methods below.
Joint pain, or polyarthralgia, involves discomfort in the joints that can be mild or severe, intermittent or persistent. Causes vary based on overall health and lifestyle, with seniors particularly vulnerable—affecting 1 in 3 individuals, primarily due to osteoarthritis.
For ongoing or severe pain, consult a healthcare professional promptly. Accurate diagnosis is crucial for targeted treatment.
What are the key symptoms?
Symptoms are straightforward to identify:
Not all symptoms occur together; they depend on the underlying cause.
Osteoarthritis, the leading cause of joint pain, involves accelerated cartilage wear in the joints. Knees are commonly affected. It's prevalent in those who are overweight, elite athletes, seniors over 70, and postmenopausal women over 55.
Types include:
No cure exists, but pain management includes medications, lifestyle changes like walking, swimming, or weight loss, and advanced cases may require prosthetic surgery.
Arthritis causes joint inflammation—acute or chronic—previously known as rheumatism. It impacts joints, ligaments, tendons, and bones, severely affecting quality of life.
Common forms:
Symptom relief comes from painkillers and anti-inflammatories; treat underlying diseases to slow progression.
Gout results from uric acid crystal deposits in joints due to hyperuricemia. Attacks cause intense inflammation, often starting in the big toe.
Seek medical care for attacks: painkillers, anti-inflammatories, or joint fluid drainage. Long-term uric acid regulation prevents recurrence.
Lupus, a chronic autoimmune disease, produces antibodies attacking healthy tissues, inflaming skin, muscles, joints, organs, and more. Flare-ups are triggered by stress, fatigue, pregnancy, or sun exposure.
Manage flares with anti-inflammatories, corticosteroids, immunosuppressants, or immunoglobulin infusions.
Scleroderma, another autoimmune condition, hardens skin and tissues, including joints, mimicking arthritis symptoms. Systemic forms affect organs like heart, lungs, and kidneys. Treatments alleviate symptoms and improve daily function.
Prevention starts with lifelong healthy habits: regular exercise, balanced weight, moderation in indulgences, daily fruits/vegetables, and ample hydration—cartilage is 75% water!
Early-stage pain may respond to osteopathy or herbal remedies; consult a doctor if it persists or worsens.